So, what’s hallux valgus? It’s a slow, progressive deformity of the big toe and it occurs in women more than men. Typically, there are around nine women for every man with a so-called bunion. There are two types of hallux valgus, one which occurs through adolescence, the other one which is most common in adults. Even though the shoes we wear can increase the misalignment, it’s mostly not the case so ladies, don’t worry about wearing heels! There are a lot of women who wear heels on a daily basis and have never experienced hallux valgus. There are two types of surgery that can help resolve this issue.
If you want to learn more about this, keep reading the article by Dr. Rayan Baalbaki.
There is no point in suffering, come and consult instead!
Heels are an essential part of the female wardrobe. But beyond appearance, do heels really cause deformities of the foot, called hallux valgus or, more often, bunions? Meeting with Dr. Rayan Baalbaki, specialist in foot surgery at the Clinique de Montchoisi in Lausanne.
What is hallux valgus?
This is a slow, progressive deformity of the big toe, better known as the “bunion”. This misalignment occurs much more frequently in women than in men: In general, there are nine women for every man with a bunion.
Does it have to do with age?
There are two types of hallux valgus: the juvenile, more constitutional type, which occurs during growth through adolescence, and the degenerative hallux valgus, which is most common in adults. So it’s true: just like osteoarthritis, hallux valgus tends to develop with age and aging of the osteoarticular structures.
However, there is no actual age limit or deformity limit – small or large – for surgery. It must be a treatment à la carte, adapted to the individual patient, according to their expectations, their quality of life, their functional requirements, their comorbidities, etc.
Do shoe heels have a direct influence on the hallux valgus deformity of the foot?
Certainly tight-fitting, narrow, pointed shoes and heels can increase the misalignment with a corresponding disposition. However, many women who wear high heels every day never get hallux valgus. We are dealing here with a multifactorial origin in which a predisposing genetic factor plays a role (e.g. Egyptian feet: the big toe is longer than the second toe; flat feet, ligament hyperlaxis, etc.). So women shouldn’t feel guilty about wearing high heels.
Can you prevent and avoid hallux valgus?
And if so, how? Yes, in any case. If you have a predisposition and the deformity develops gradually, the first thing you need to do is adjust your shoes. I always tell my patients that it is easier to fit the shoe to the foot than it is to fit the foot to the shoe. Therefore, it is advisable to wear wide, comfortable shoes, ideally with an orthopedic insole from a podiatrist or orthopedic shoemaker. There are also inter-toe braces that are placed between the toes to prevent them from crossing over.
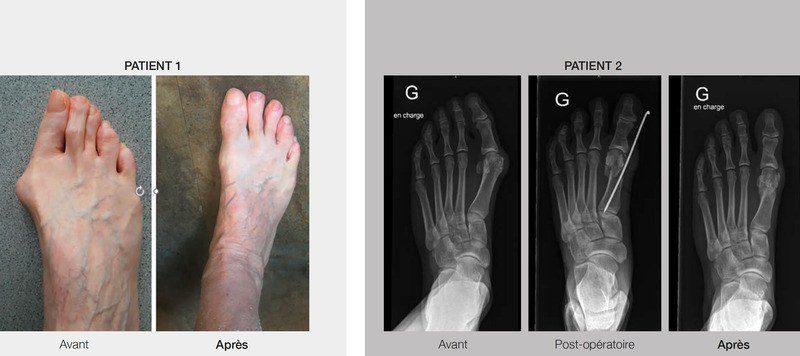

When is an operation necessary?
Surgery is indicated and recommended for deformities that are annoying on a daily basis. In fact, some women observe an increase in their deformity or disability due to pain despite having fitted shoes and tailor-made soles. In these cases, it is recommended not to wait for the deformity to worsen and worsen, but to undergo surgical treatment.
What does an intervention look like?
There are two main types of surgery: The oldest, traditional surgical procedure is open, but the more tissue-conserving percutaneous or minimally invasive surgery (MIS, abbreviation for Minimally Invasive Surgery) has been gradually gaining ground since the early 2000s.
One can even speak of a “new wave” sweeping through the world of foot and ankle surgery. “The Tsunami” of percutaneous surgery.
It should be noted that percutaneous surgery is still difficult and requires special training, as bone and tendon operations are performed through millimeter-sized skin incisions.
There are numerous advantages associated with these new techniques: the operation time is shorter, the surgery is less aggressive, scars are almost imperceptible (minimal) and the patients experience much less pain or none at all (in almost 20% of the cases). But be careful, the pain threshold is different for everyone.
Since the aggression on the tissue is reduced, the patients recover faster: They can walk with a special orthopedic shoe immediately after the operation, which they have to wear for four to six weeks.
Thorough postoperative follow-up care is of paramount importance for positive development.



![CH12768_BANNER-MANCASSOLA-980x180-EN[1]](https://rang-group.ch/wp-content/uploads/2021/05/CH12768_BANNER-MANCASSOLA-980x180-FR1.png?v=3762)
